New Hampshire Survey Respondents Struggle to Afford High Health Care Costs; Worry about Affording Health Care in the Future; Support Government Action Across Party Lines
Key Findings
A survey of more than 1,300 New Hampshire adults, conducted from March 26 to May 14, 2024,
found that:
- Over 3 in 5 (71%) experienced at least one health care affordability burden in the past year;
- Over 4 in 5 (83%) worry about affording health care in the future;
- Over 3 in 5 (69%) of all respondents delayed or went without health care due to cost in the last twelve months;
- Low-income respondents and those with disabilities had higher rates of going without care due to cost and incurring medical debt, depleting savings, and/or sacrificing basic needs due to medical bills; and
- Across party lines, respondents express strong support for government-led solutions.
A Range of Health Care Affordability Burdens
Like many Americans, New Hampshire adults experience hardship due to high health care costs. Overall,
seven out of ten (71%) respondents experienced one or more of the following health care affordability
burdens in the prior 12 months:
1) Being Uninsured Due to High Costs
Almost half (47%) of uninsured respondents cited "too expensive" as the main reason for not having
health insurance, far exceeding other reasons like "don't need it" and "don't know how to get it." In
addition, 49% of respondents without dental insurance and 41% those without vision insurance cited cost
as the main reason for not having coverage.
2) Delaying or Going Without Health Care Due to Cost
Over two-thirds (69%) of all respondents reported delaying or going without health care during the prior
12 months due to cost:
- 32%-Skipped needed dental care
- 29%—Delayed going to the doctor or having a procedure done
- 29%—Skipped a recommended medical test or treatment
- 25%—Cut pills in half, skipped doses of medicine or did not fill a prescription1
- 20%—Avoided going to the doctor or having a procedure done altogether
- 18%—Skipped needed vision services
- 17%—Had problems getting mental health care or addiction treatment2
- 8%-Skipped needed hearing services
- 6%—Skipped or delayed getting a medical assistive device
Moreover, respondents most frequently cited cost as the reason for them or their family members not
getting care in the last year (25%), followed by not being able to get an appointment (23%), exceeding a
host of other barriers such as getting time off work, transportation, or childcare.
3) Struggling to Pay Medical Bills
Other times, respondents got the care they needed but experienced a cost burden due to the resulting
medical bill(s). Over two in five (41% of) respondents reported experiencing one or more of these
struggles to pay their medical bills:
- 17%—Were contacted by a collection agency
- 14%—Used up all or most of their savings
- 13%—Were unable to pay for basic necessities like food, heat, or housing
- 13%—Racked up large amounts of credit card debt
- 10%-Borrowed money, got a loan, or another mortgage on their home
- 10%—Were placed on a long-term payment plan
- 2%—Asked for donations/crowdfunding (e.g., GoFundMe campaigns)
High Levels of Worry About Affording Health Care in the Future
New Hampshire respondents also exhibit high levels of worry about affording health care in the future.
Over four in five (83%) reported being "worried" or "very worried" about affording some aspect of health
care in the future, including:
- 70%—Cost of nursing home or home care services
- 65%—Medical costs when elderly
- 63%—Health insurance will become unaffordable
- 62%—Medical costs in the event of a serious illness or accident
- 55%—Cost of dental care
- 53%—Prescription drugs will become unaffordable
- 46%—Cost of needed vision services
- 45%—Cost of needed hearing services
While two of the most common worries-affording the cost of nursing home or home care services and
medical costs when elderly—are applicable predominantly to an older population, they were most
frequently reported by younger respondents. Respondents ages 18-54 reporting higher worries of paying
for medical costs when elderly and respondents ages 35-64 report higher worries of affording the cost of
a nursing home or home care services. This finding suggests that New Hampshire respondents may be
worried about affording the cost of care for both aging relatives in addition to themselves.
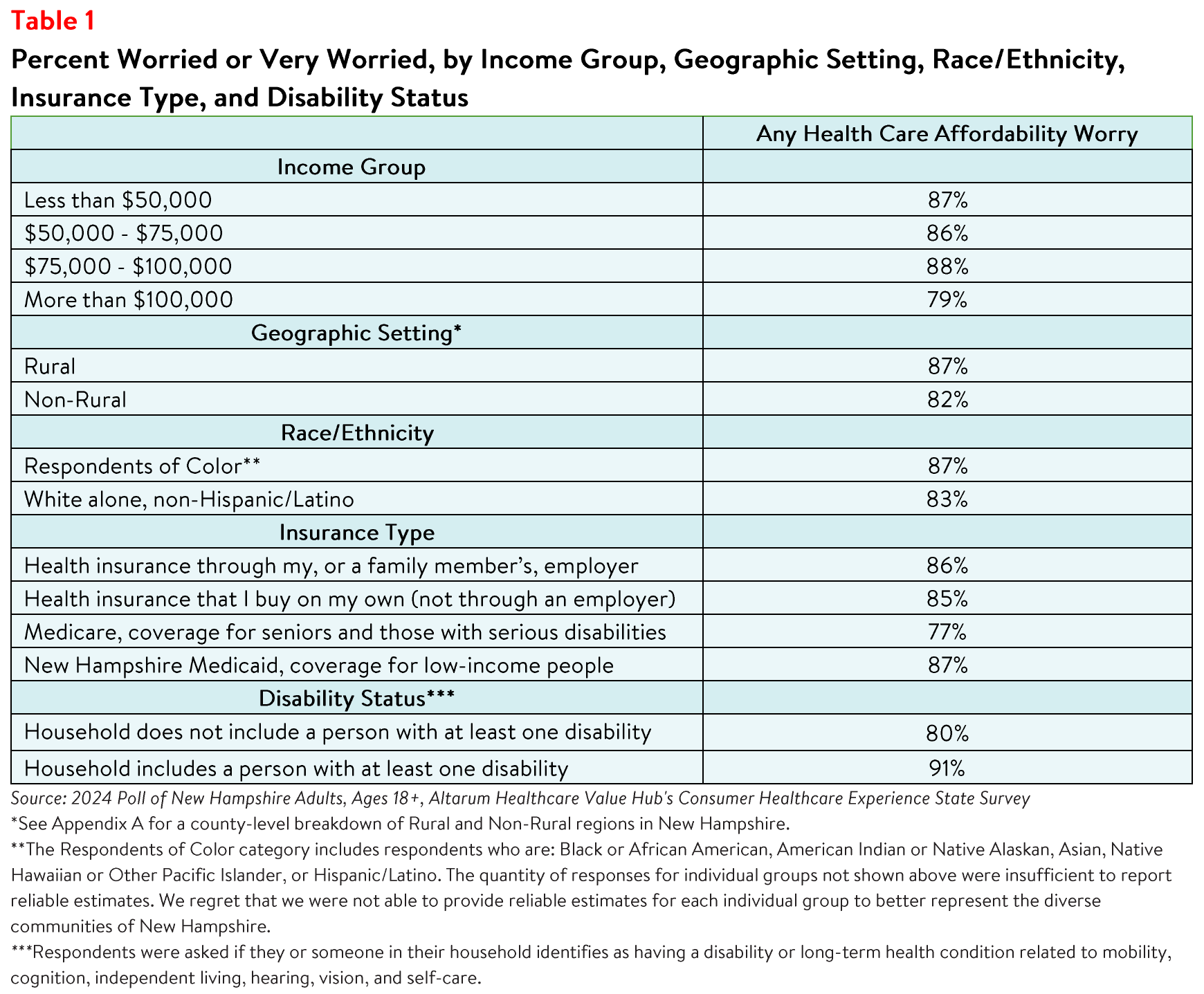
Worry about affording health care was highest among respondents living in lower-income households,
among those living in households with a person with a disability, and those living in rural areas (see Table 1). Overall, 87% of respondents with household incomes less than $100,000 a year reported worrying about affording some aspect of coverage or care in the past year, however 79% of those earning over $100,000 per year were also worried.3 Most New Hampshire respondents of all incomes, geographic settings, races, ethnicities, insurance types, and levels of ability were somewhat or very concerned.
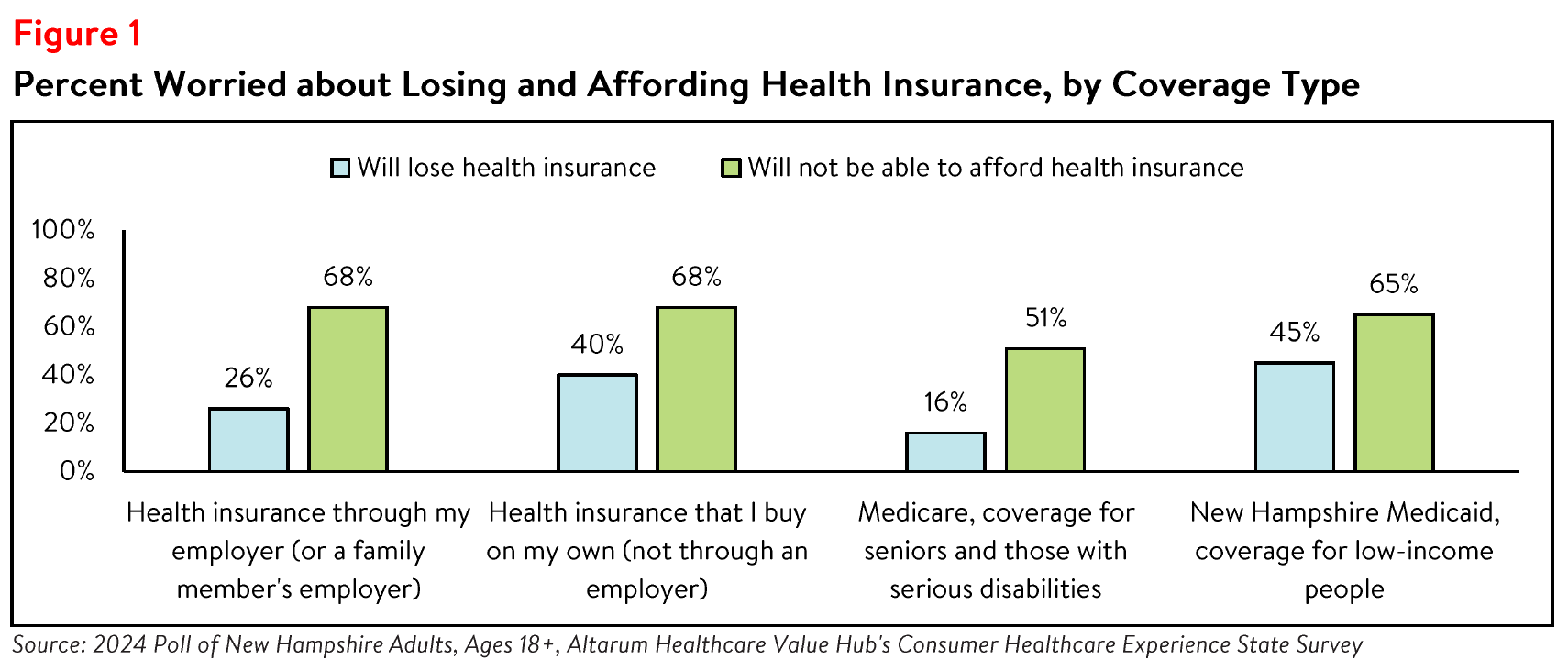
Concern that health insurance will become unaffordable is also prevalent among many New Hampshire
respondents. By insurance type, respondents with Medicaid coverage, coverage that they have through an employer, and coverage that they purchased on their own most frequently reported worrying about
affording coverage (see Figure 1). Still, over half (51%) of those with Medicare coverage reported worrying about affording coverage.
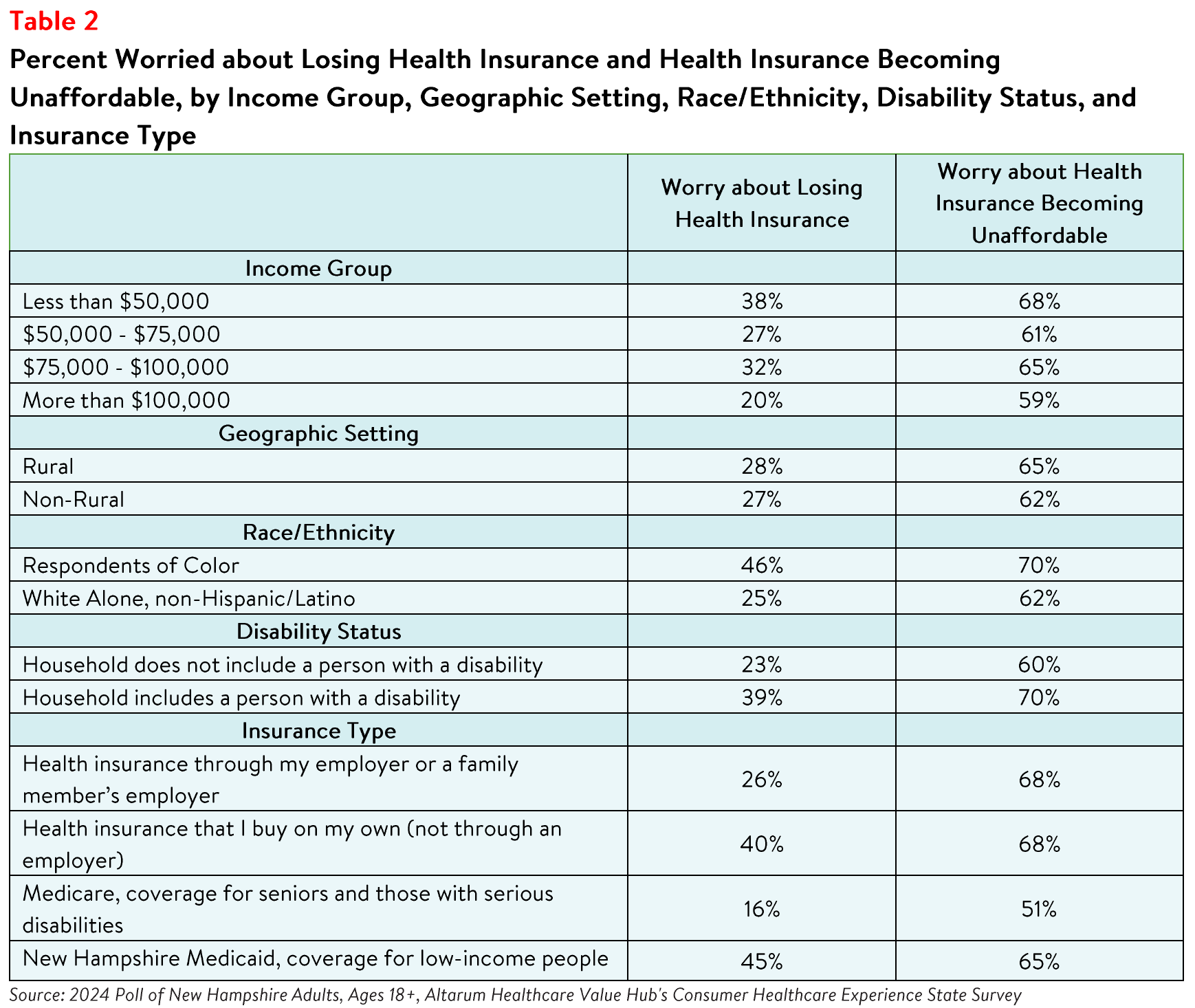
Respondents with household incomes below $50,000 per year reported the highest rates of worry about
losing coverage and not being able to afford coverage in the future (see Table 2). Respondents living in
households with a person with a disability reported higher rates of being concerned about losing health
insurance than those living in a household without a person with a disability. Respondents living in rural
areas reported a higher rate of worry about affording insurance in the future compared to residents in
non-rural areas.
Concerns about affording coverage exceeded worries about losing coverage across all income groups,
disability statuses, geographic settings, races/ethnicities, and coverage types.
Differences in Health Care Affordability Burdens
The survey also revealed differences in how New Hampshire respondents experience health care
affordability burdens by income level, age, geographic setting, race/ethnicity, and disability status.
Income and Age
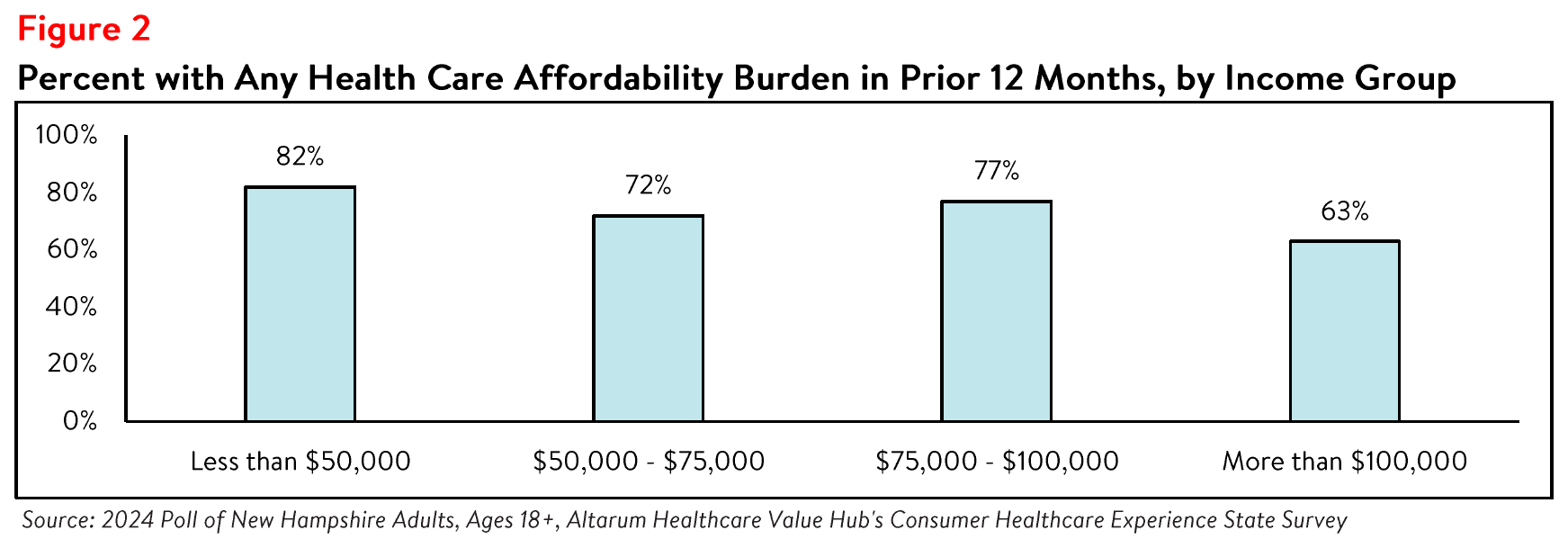
Unsurprisingly, respondents at the lowest end of the income spectrum most frequently reported
experiencing one or more health care affordability burdens, with over four out of five (82%) of those
earning less than $50,000 per year reporting struggling to afford some aspect of coverage or care in the
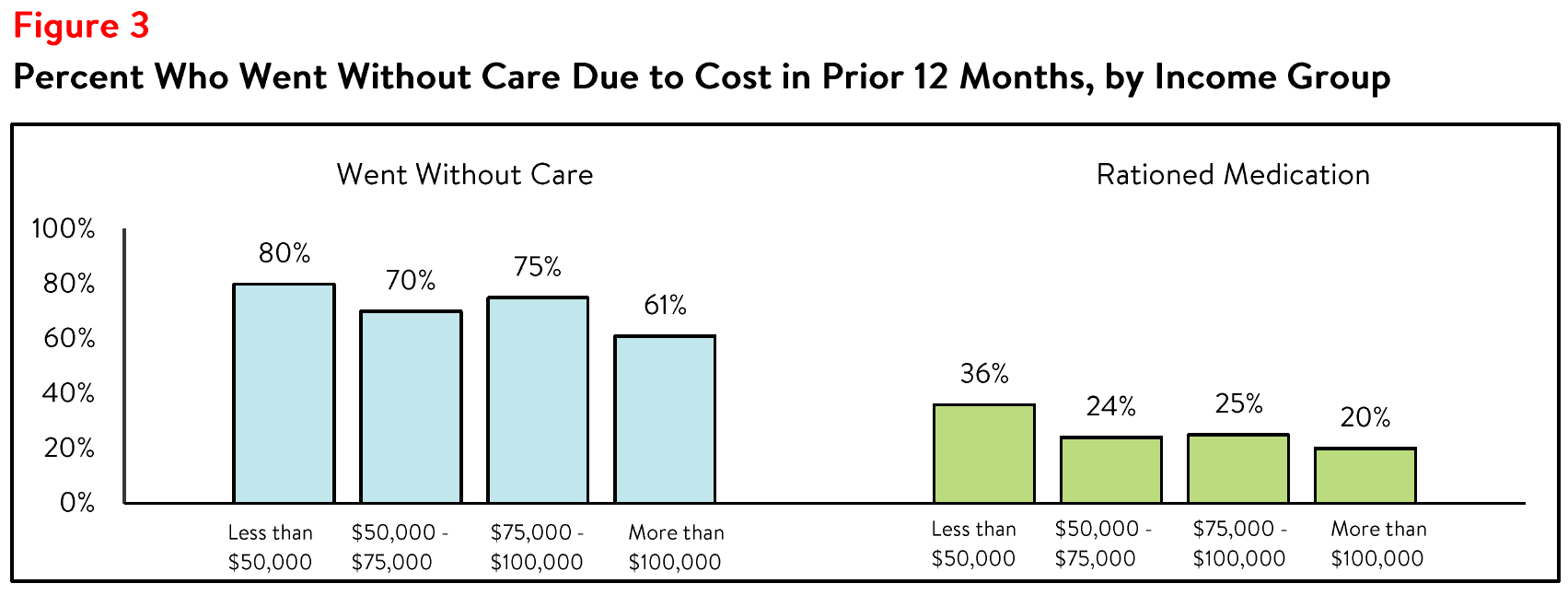
past 12 months (see Figure 2). This may be due, in part, to respondents in this income group reporting higher rates of going without care and rationing their medication due to cost (see Figure 3).
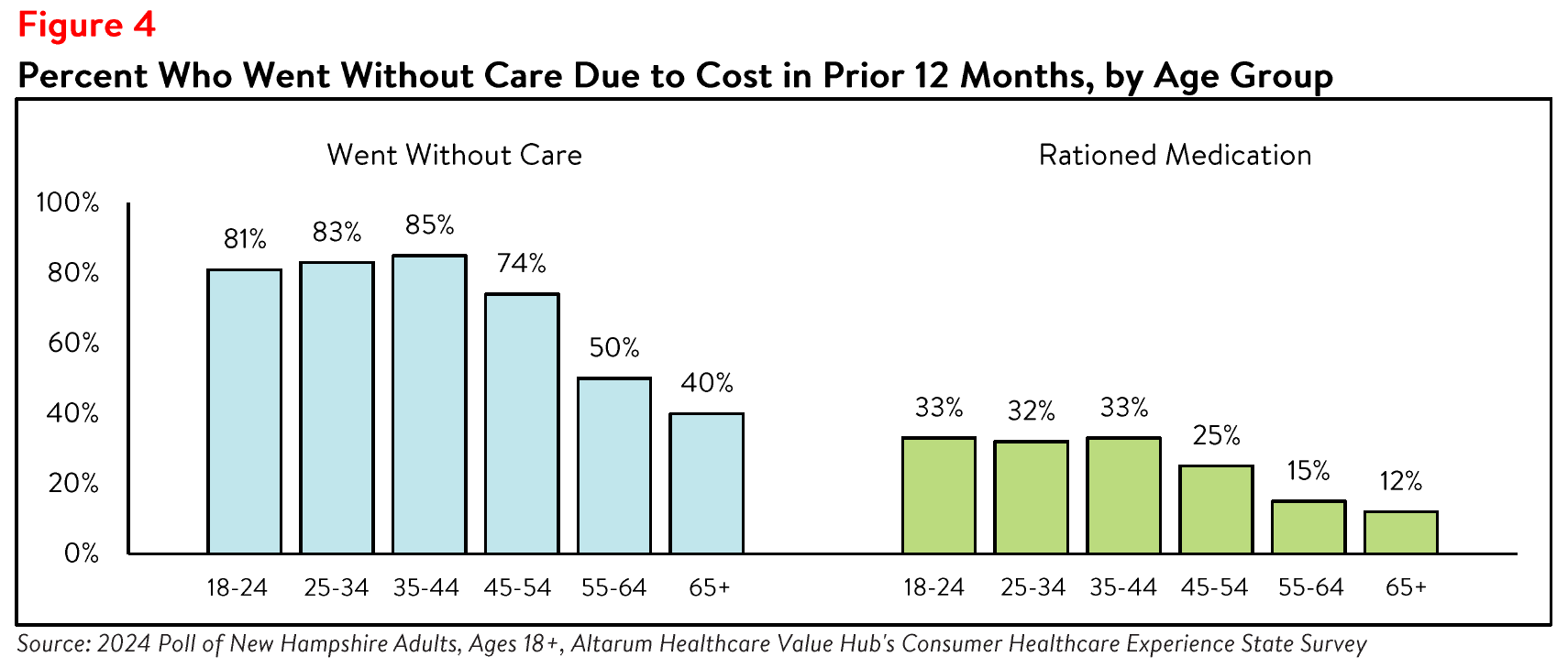
Further analysis found that New Hampshire respondents ages 18-44 reported higher rates of going
without care due to cost than respondents ages 45 and older (see Figure 4). Respondents ages 18-44 also most frequently reported rationing medication due to cost compared to other age groups.
Disability
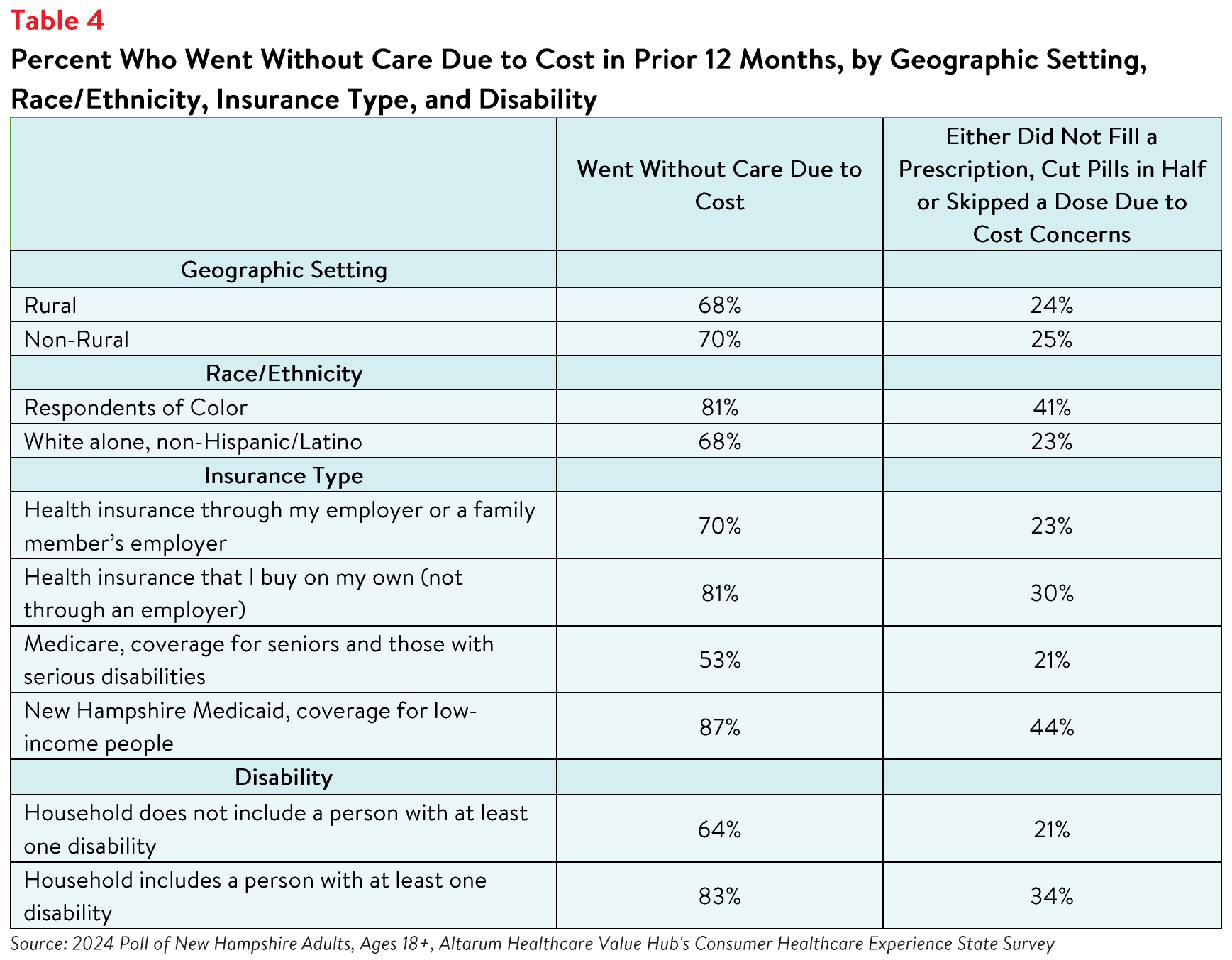
Respondents living in households with a person with a disability reported the highest rates of going
without care and rationing medication due to cost in the past 12 months. Over eight in ten (83% of)
respondents in this group reported going without some form of care and 34% reported rationing
medication, compared to 64% and 21% of respondents living in households without a person with a
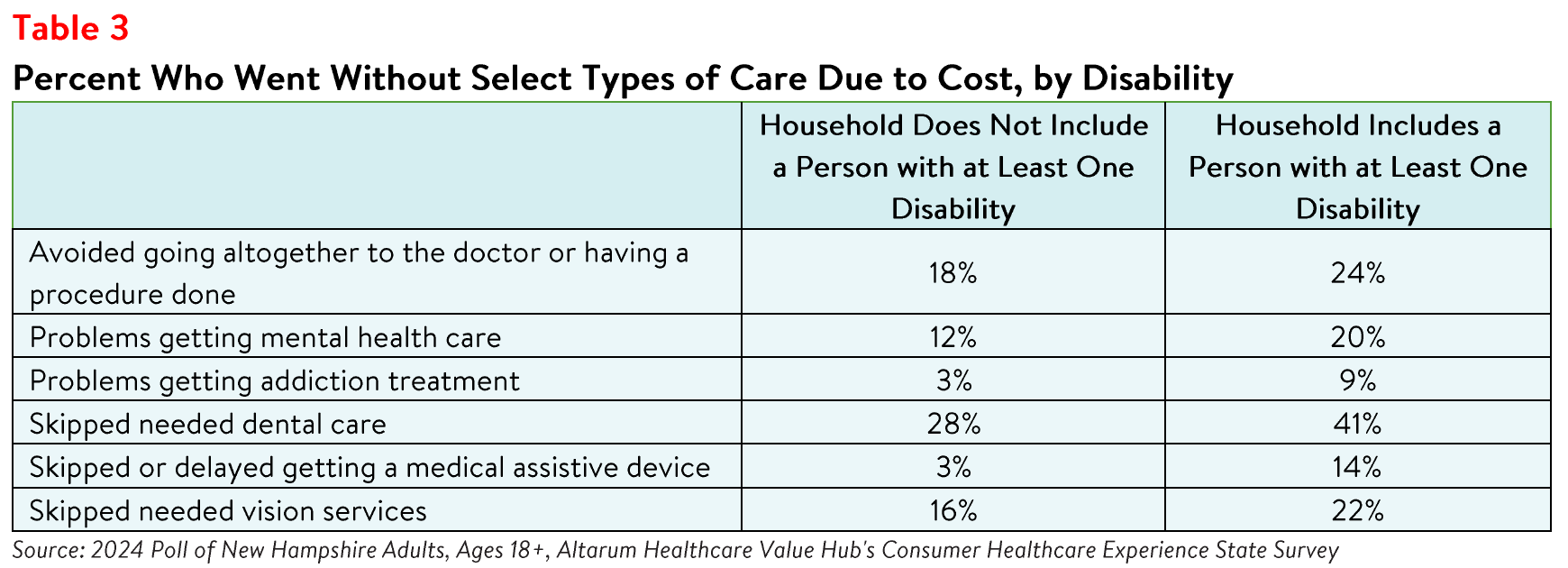
disability, respectively (see Table 4). Respondents living in households with a person with a disability also
more frequently reported delaying or skipping getting mental health care, addiction treatment, and dental
care, among other health care services, than those in households without a person with a disability due to
cost concerns (see Table 3).
Those with disabilities also face health care affordability burdens unique to their disabilities—14% of
respondents with a disabled household member reported delaying getting a medical assistive device such
as a wheelchair, cane/walker, hearing aid, or prosthetic limb due to cost. Just 3% of respondents without a
person with a disability in their household (who may have needed such tools temporarily or may not
identify as having a disability) reported this experience.
Insurance Type
People with different types of insurance navigate the health care system in varying ways. Those with
private insurance may face higher premiums and out-of-pocket costs, while individuals enrolled in
Medicaid or Medicare generally have lower costs but may encounter limited provider options, greater
restrictions around covered services, and longer wait times for services.
Respondents with New Hampshire Medicaid coverage reported the highest rates of going without care
due to cost and rationing medication, followed by respondents with private insurance purchased
independently (see Table 4). Still, over half (53%) of respondents with Medicare coverage also went
without care due to cost in the twelve months prior to taking the survey.
Race and Ethnicity
New Hampshire respondents of color reported higher rates of rationing medication and forgoing care
than white alone, non-Hispanic/Latino respondents. There are a variety of potential consequences related
to postponing health care and medication rationing, highlighting the importance of addressing costrelated
barriers to address health disparities.
Eighty-one percent of respondents of color reported going without care due to cost in the past twelve
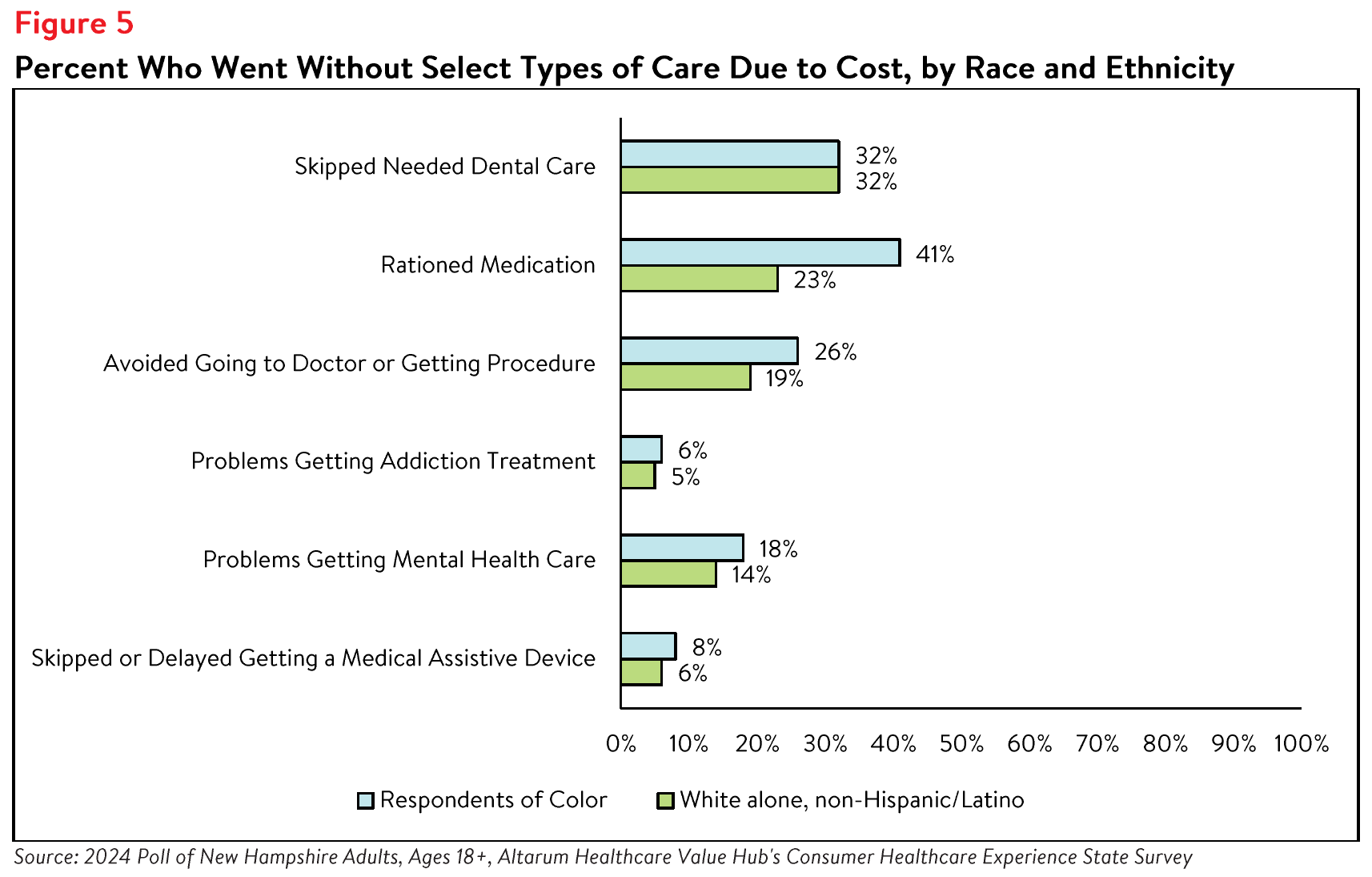
months compared to 68% of white alone, non-Hispanic/Latino respondents (see Table 4). Further analysis
showed that respondents of color also reported higher rates of challenges receiving mental health care
and skipping needed dental care (see Figure 5).
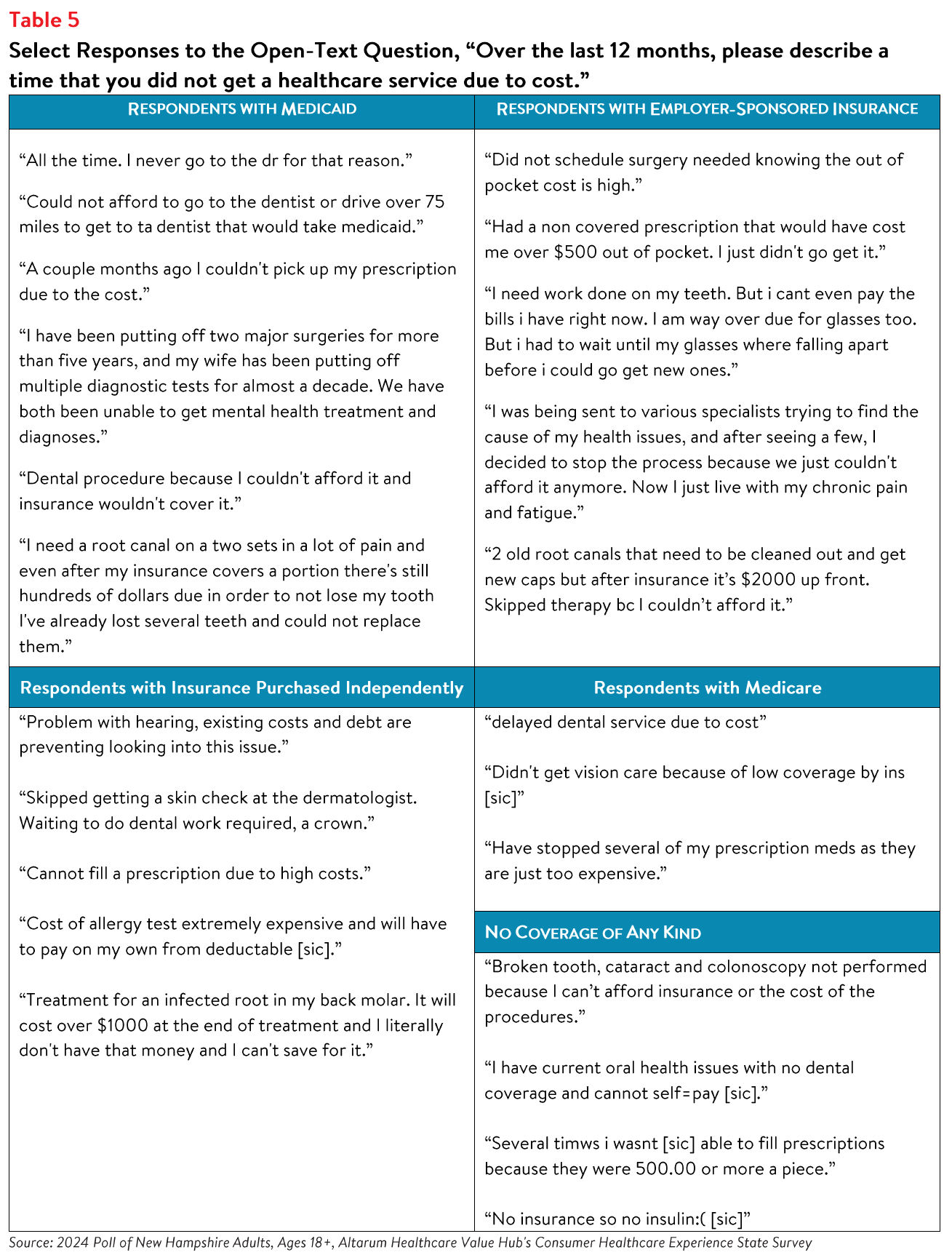
In an effort to explore the impact high health costs have on individuals, respondents were also asked to
describe a time that they were unable to get health care due to cost (see Table 5). These anecdotes
highlight the nature of affordability challenges, underscore the impact of health care costs on individuals,
and emphasize the need for solutions to reduce financial barriers to health care.

Encountering Medical Debt
In the absence of affordable care options, individuals may find themselves burdened by medical costs. To
explore the impact of unaffordable medical care, survey participants were asked whether they have had to
do any of the following due to the cost of medical bills in the past twelve months: use up all or most of
their savings; sacrifice basic necessities, such as food, heat, or housing; borrow money, get a loan or take
out another mortgage; use a crowdfunding platform to solicit donations; interact with a collections
agency; go into credit card debt; be placed on a long-term payment plan; or declare bankruptcy.
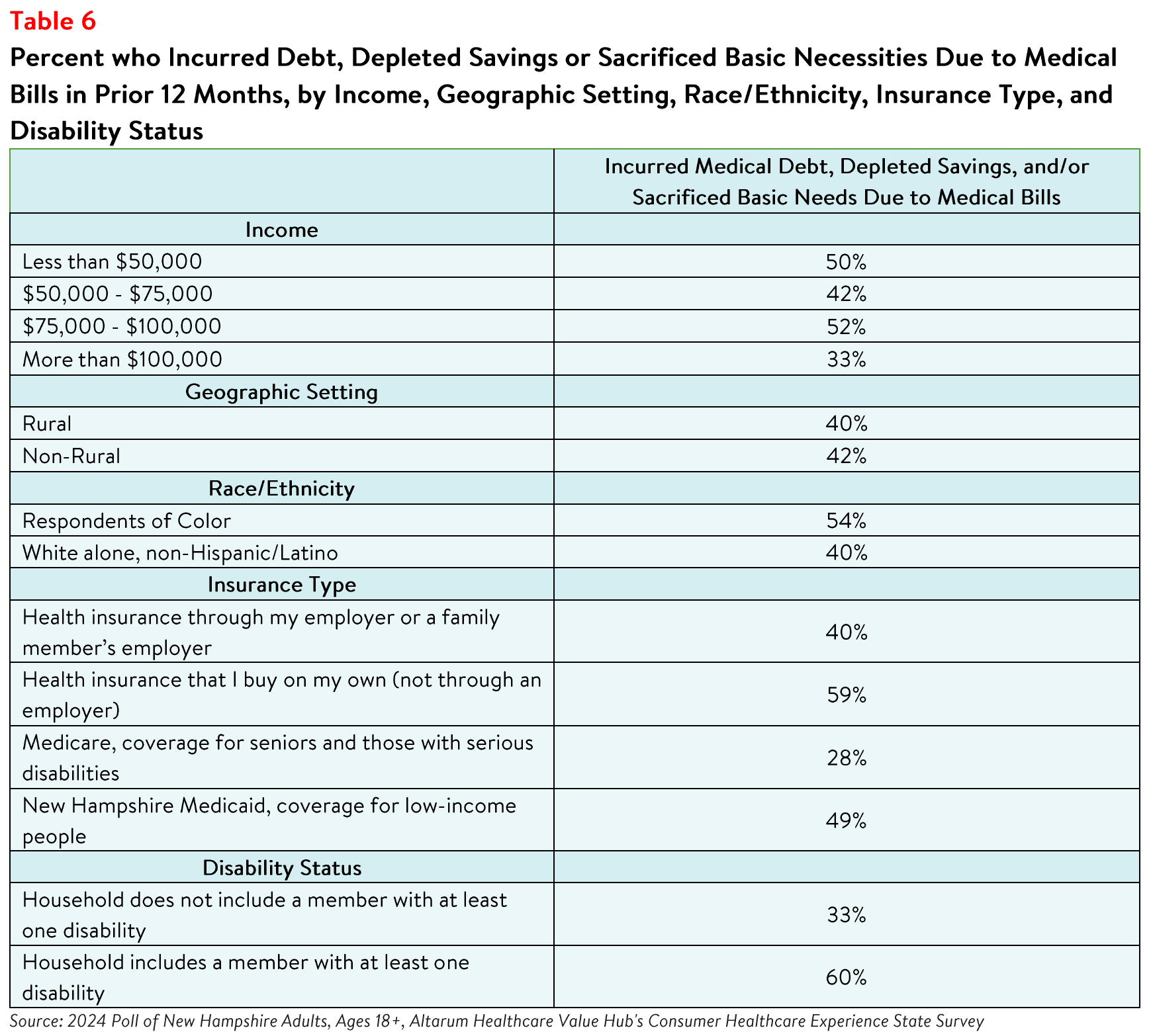
The survey results revealed that 54% of respondents of color reported going into debt, depleting savings,
or going without other needs due to medical bills, compared to 40% of white alone, non-Hispanic/Latino
respondents (see Table 6). The rate of financial burden is even higher for respondents who have or live
with a person with a disability, with three-fifths (60%) reporting going into debt or going without other
needs due to medical bills, compared to 33% of respondents without a disabled household member. In
addition, respondents with health insurance bought independently reported the highest rate of the above
financial burdens due to medical bills (59%) compared to respondents with all other insurance types.
Impact and Worry Related to Hospital Consolidation*
In addition to the above health care affordability burdens, a small share of New Hampshire respondents
were negatively impacted by health system consolidation. From 2020 to 2022, there were 6 changes in
ownership involving hospitals through mergers, acquisitions, or changes of ownership (CHOW) in New
Hampshire.4,5 New Hampshire requires that the State Attorney General be notified and is accompanied
with a waiting period for health care-specific nonprofit transactions.6
In the past year, 36% of respondents reported that they were aware of a merger or acquisition in their
community—of those respondents, 17% reported that they or a family member were unable to access their preferred health care organization because of a merger that made their preferred organization out-of network. Out of those who reported being unable to access their preferred health care provider due to a
merger:
- 62% delayed or avoided going to the doctor or having a procedure done because they could no longer access their preferred health care organization due to a merger
- 35% skipped recommended follow-up visits due to a merger
- 22% skipped filling a prescription medication due to a merger
- 19% changed their preferred doctor or hospital to one that is in-network
Out of those who reported that the merger caused an additional burden for them or their families, the top
three most frequently reported issues were:
- 42%—The merger created an added wait time when searching for a new provider
- 24%—The merger created an added financial burden
- 16%—The merger created a gap in the continuity of my care
While a smaller portion of respondents reported being unable to access their preferred health care
organization because of a merger, 54% of respondents who reported not being impacted by a health care
merger reported that, if there were mergers happening in their community, they would be somewhat, moderately, or very worried about the impacts of mergers in their health care organizations.
When asked about their largest concern respondents most frequently reported:
- 31%—I'm concerned I will have fewer choices of where to receive care
- 27%—I'm concerned my doctor may no longer be covered by my insurance
- 20%—I'm concerned I will have to pay more to see my doctor
- 12%—I'm concerned I will have a lower quality of care
- 9%—I'm concerned I will have to travel farther to see my doctor
Dissatisfaction with the Health System and Support for Change
In light of New Hampshire respondents' health care affordability burdens and concerns, it is not surprising
that they are dissatisfied with the health system:
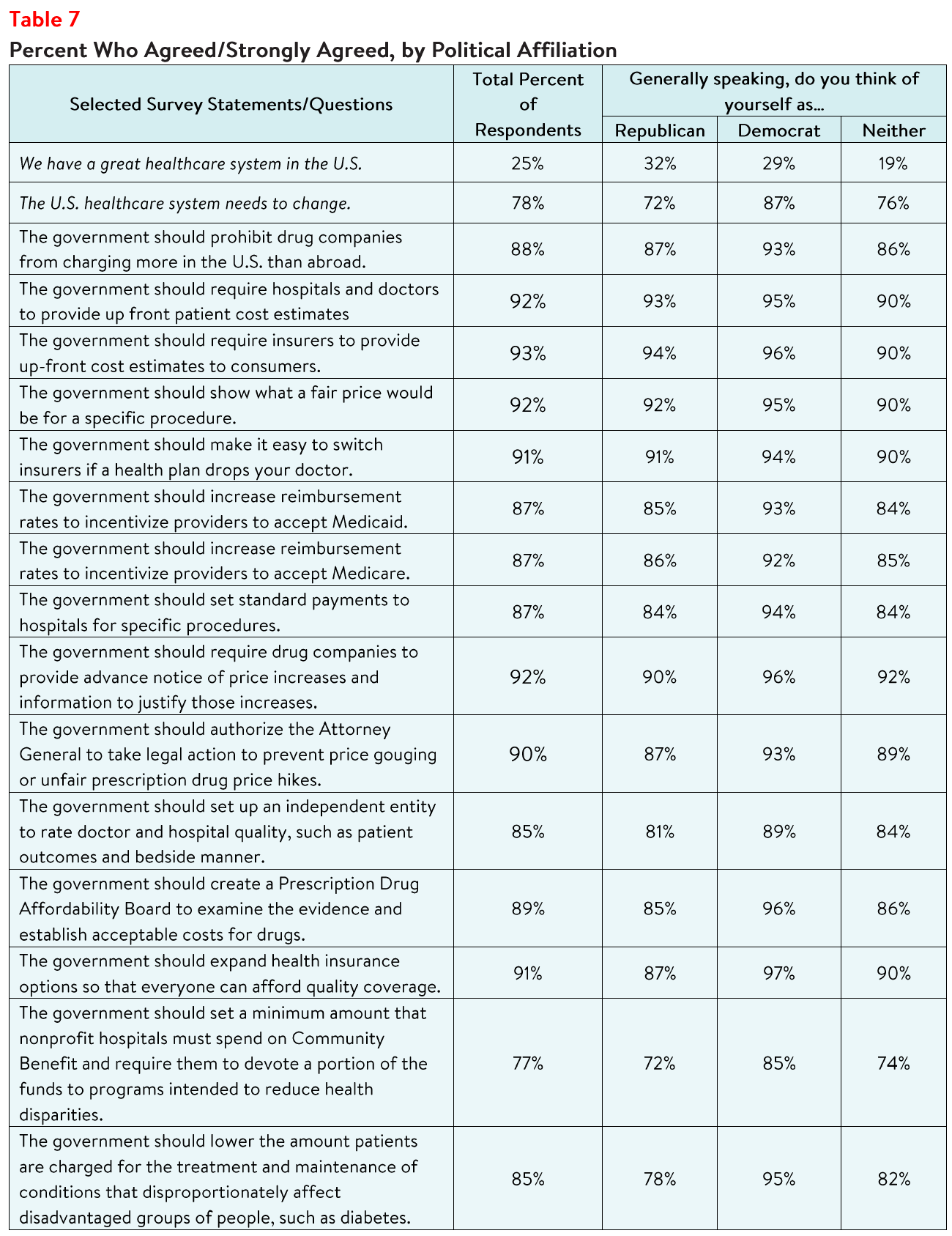
- Just 25% agreed or strongly agreed that "we have a great healthcare system in the U.S.,"
- While 78% agreed or strongly agreed that "the system needs to change."
To investigate further, the survey asked about both personal and governmental actions to address health
system problems.
Personal Actions
New Hampshire respondents see a role for themselves in addressing health care affordability. When asked about specific actions they could take:
- 54% of respondents reported researching the cost of a drug beforehand, and
- 81% said they would be willing to switch from a brand name to an equivalent generic drug if given the chance.
When asked to select the top three personal actions they felt would be most effective in
addressing health care affordability (out of ten options), the most common responses were:
- 62%—Take better care of my personal health
- 37%—Research treatments myself before going to the doctor
- 29%—Do more to compare doctors on cost and quality before getting services
- 26%—Write to or call my state representative asking them to take action on high health care prices and lack of affordable coverage options
- 28%—There is not anything I can do personally to make our health system better
Government Actions
But far and away, New Hampshire respondents see government as the key stakeholder that needs to act
to address health system problems. Moreover, addressing health care problems is one of the top priorities
that respondents want their elected officials to work on.
At the beginning of the survey, respondents were asked what issues the government should address in the upcoming year. The top vote getters were:
- 44%—Health care
- 43%—Economy/Joblessness
- 40%-Affordable Housing
When asked about the top three health care priorities the government should work on, the top vote getters were:
- 54%—Address high health care costs, including prescription drugs
- 36%—Preserve consumer protections preventing people from being denied coverage or charged more for having a pre-existing medical condition
- 34%—Improve Medicare, coverage for seniors and those with serious disabilities
- 29%—Get health insurance to those who cannot afford coverage
Of 15 options, New Hampshire respondents believe the reason for high health care costs is unfair prices
charged by powerful industry stakeholders:
- 80%—Drug companies charging too much money
- 76%—Insurance companies charging too much money
- 69%—Hospitals charging too much money
When it comes to tackling costs, respondents endorsed a number of strategies, including:
- 93%—Require insurers to provide up-front cost estimates to consumers
- 92%—Show what a fair price would be for specific procedures
- 92%—Cap out-of-pocket costs for life-saving medications, such as insulin
- 92%—Require drug companies to provide advanced notice of price increases and information to justify those increases
- 92%—Require hospitals and doctors to provide up-front cost estimates to consumers
- 91%—Make it easy to switch insurers if a health plan drops your doctor
- 91%—Expand health insurance options so that everyone can afford quality coverage
- 90%—Authorize the Attorney General to take legal action to prevent price gouging or unfair prescription drug price hikes
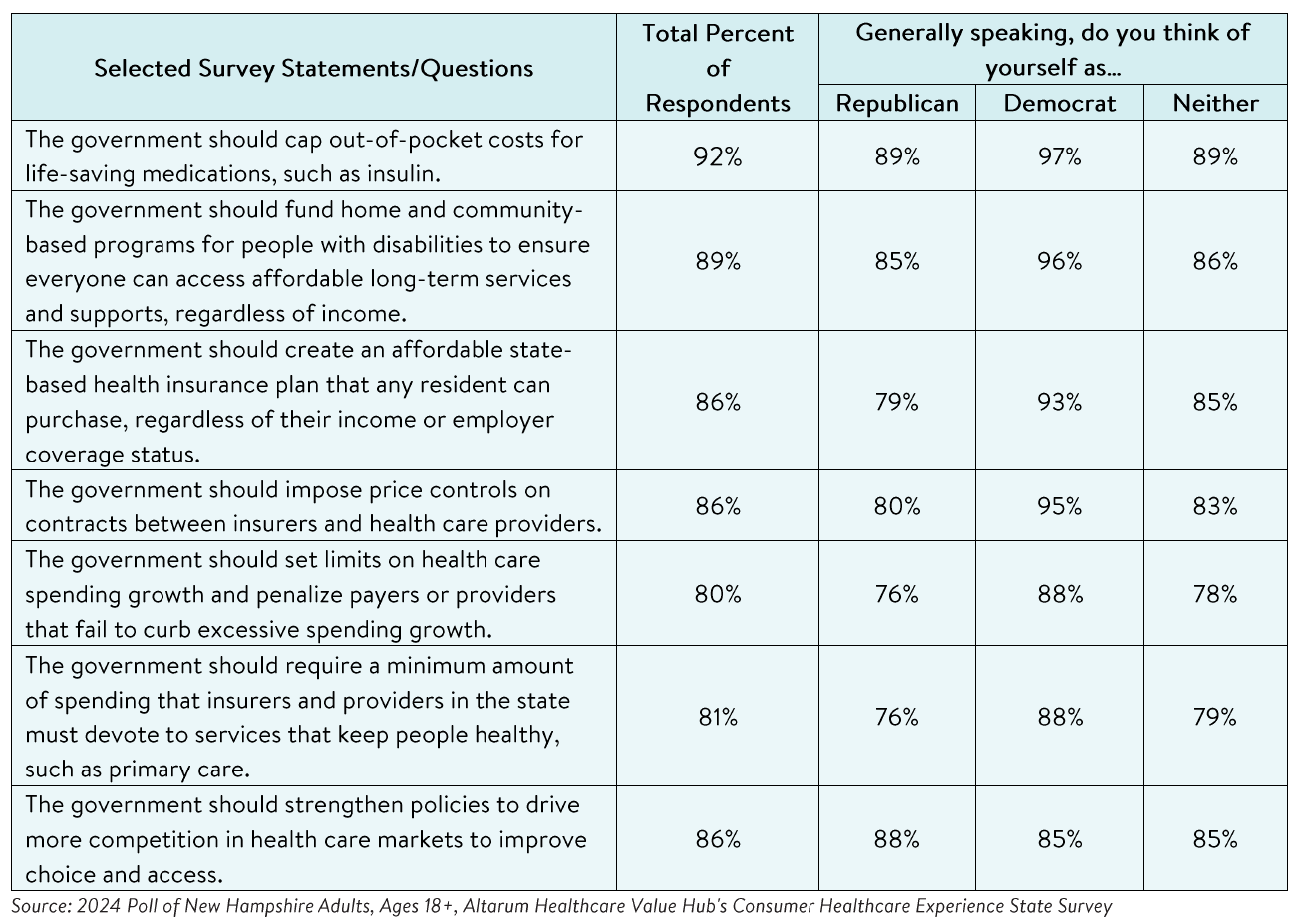
Support for Action Across Party Lines
There is also support for change regardless of respondents' political affiliation (see Table 7).
The high burden of health care affordability, along with high levels of support for change, suggest that
elected leaders and other stakeholders need to make addressing this consumer burden a top priority.
Moreover, the COVID crisis has led state residents to take a hard look at how well health systems are
working for them, with strong support for a wide variety of actions. Annual surveys can help
assess whether progress is being made.
Notes
- Nineteen percent (19%) did not fill a prescription and 12% cut pills in half or skipped doses of medicine due to cost.
- Fifteen percent (15%) had problems getting mental health care and 5% had problems getting addiction treatment.
- Median household income in New Hampshire was $90,845 (2018-2022). U.S. Census, Quick Facts. Retrieved from: U.S. Census Bureau QuickFacts, U.S. Census Bureau QuickFacts: New Hampshire.
- Centers for Medicare and Medicaid Services. (2023). Hospital Change of Ownership. Retrieved August 23, 2023, from https://data.cms.gov/provider-characteristics/hospitals-and-other-facilities/hospital-change-of-ownership.
- A CHOW typically occurs when a Medicare provider has been purchased (or leased) by another organization. The CHOW results in the transfer of the old owner's identification number and provider agreement (including any Medicare outstanding debt of the old owner) to the new owner...An acquisition/merger occurs when a currently enrolled Medicare provider is purchasing or has been purchased by another enrolled provider. Only the purchaser's CMS Certification Number (CCN) and tax identification number remain. Acquisitions/mergers are different from CHOWs. In the case of an acquisition/merger, the seller/former owner's CCN dissolves. In a CHOW, the seller/former owner's CCN typically remains intact and is transferred to the new owner. A consolidation occurs when two or more enrolled Medicare providers consolidate to form a new business entity. Consolidations are different from acquisitions/mergers. In an acquisition/merger, two entities combine but the CCN and tax identification number (TIN) of the purchasing entity remains intact. In a consolidation, the TINs and CCN of the
consolidating entities dissolve and a new TIN and CCN are assigned to the new, consolidated entity. Source: Missouri Department of Health and Senior Services, Change of Ownership Guidelines—Medicare/State Certified Hospice. Retrieved August 23, 2023, from https://health.mo.gov/safety/homecare/pdf/CHOW-Guidelines-
StateLicensedHospice.pdf#:—:text.Acquisitions%2Fmergers%20are%20different%20from%20CHOWs.%20In%20the%20cas
e,providers%20consolidate%20to%20form%20a%20new%20business%20entity. - The Source on Healthcare Price and Competition, Merger Review, Retrieved June 27, 2024 from
https://sourceonhealthcare.org/market-consolidation/merger-review/
Methodology
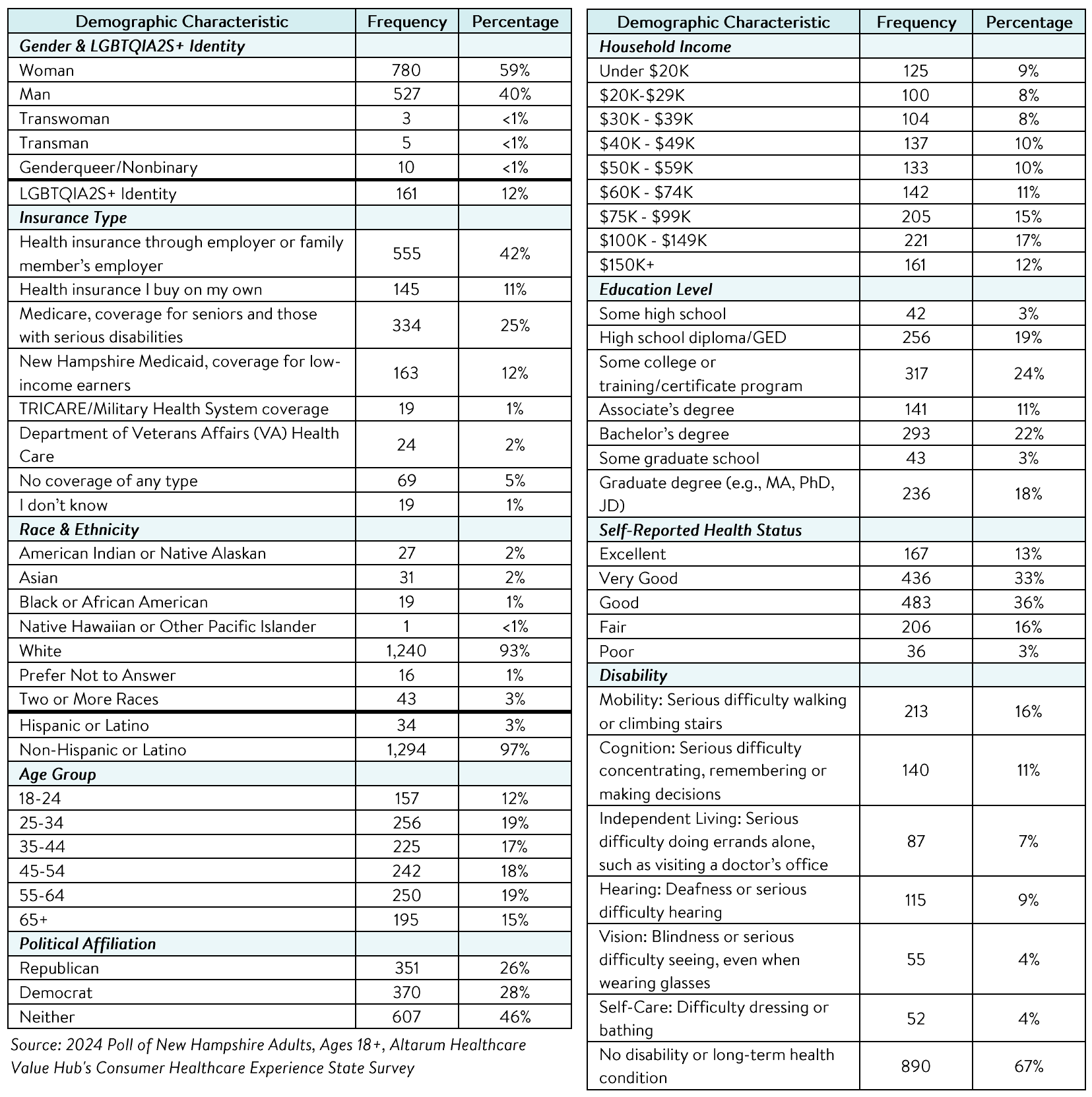
Altarum's Consumer Healthcare Experience State Survey (CHESS) is designed to elicit respondents' views on a wide range of health system issues, including confidence using the health system, financial burden and possible policy solutions. This survey, conducted from March 26 to May14, 2024, used a web panel from Dynata with a demographically balanced sample of approximately 1,500 respondents who live in New Hampshire. Information about Dynata's recruitment and compensation methods can be found here. The survey was conducted in English or Spanish and restricted to adults ages 18 and older. Respondents who finished the survey in less than half the median time were excluded from the final sample, leaving 1,328 cases for analysis. After those exclusions, the demographic composition of respondents was as follows, although not all demographic information has complete response rates: